Disease Center.

Chickenpox is a common illness that causes an itchy rash and red spots or blisters (pox) all over the body. It is most common in children, but most people will get chickenpox at some point in their lives if they have not had the chickenpox vaccine.
Chickenpox usually isn't serious in healthy children. But it can cause problems for pregnant women, newborns, teens and adults, and people who have immune system problems that make it hard for the body to fight infection.
After you have had chickenpox, you are not likely to get it again. But the virus stays in your body long after you get over the illness. If the virus becomes active again, it can cause a painful viral infection called shingles.
Chickenpox is caused by the varicella-zoster virus. It can spread easily. You can get it from an infected person who sneezes, coughs, or shares food or drinks. You can also get it if you touch the fluid from a chickenpox blister.
A person who has chickenpox can spread the virus even before he or she has any symptoms. Chickenpox is most easily spread from 2 to 3 days before the rash appears until all the blisters have crusted over.
You are at risk for chickenpox if you have never had the illness and have not had the chickenpox vaccine. If someone you live with gets chickenpox, your risk is even higher because of the close contact.

The first symptoms of chickenpox often are a fever, a headache, and a sore throat. You or your child may feel sick, tired, and not very hungry. The chickenpox rash usually appears about 1 or 2 days after the first symptoms start. Some children get the chickenpox rash without having a fever or other early symptoms.
It usually takes 14 to 16 days to get the symptoms of chickenpox after you have been around someone with the virus. This is called the incubation period.
After a chickenpox red spot appears, it usually takes about 1 or 2 days for the spot to go through all its stages. This includes blistering, bursting, drying, and crusting over. New red spots will appear every day for up to 5 to 7 days.
You or your child can go back to work, school, or day care when all blisters have crusted over. This is usually about 10 days after the first symptoms start.

Your doctor will ask you about your symptoms and will examine you. This usually gives your doctor enough information to find out if you have chickenpox
Ringworm of the skin is an infection caused by a fungus. Ringworm can affect skin on your body (tinea corporis), scalp (tinea capitis), groin area (tinea cruris, also called jock itch), or feet (tinea pedis, also called athlete's foot).
Although the name suggests so, Ringworm is not caused by a worm. It is caused by a fungus. The kinds of fungi that cause ringworm live and spread on the top layer of the skin and on the hair. They grow best in warm, moist areas, such as locker rooms and swimming pools, and in skin folds.
Ringworm is contagious. It spreads when you have skin-to-skin contact with a person or animal that has it. It can also spread when you share things like towels, clothing, or sports gear.

Ringworm of the skin usually causes a very itchy rash. It often makes a pattern in the shape of a ring, but not always. Sometimes it is just a red, itchy rash. Jock itch is a rash in the skin folds of the groin. It may also spread to the inner thighs or buttocks.
Ringworm of the hand looks like athlete's foot. The skin on the palm of the hand gets thick, dry, and scaly, while skin between the fingers may be moist and have open sores.
If you have a ring-shaped rash, you very likely have ringworm. Your doctor will be able to tell for sure. He or she will probably look at a scraping from the rash under a microscope to check for the ringworm fungus
Most ringworm of the skin can be treated at home with creams you can buy without a prescription. Your rash may clear up soon after you start treatment, but it’s important to keep using the cream for as long as the label or your doctor says. This will keep the infection from coming back. If the cream doesn't work, your doctor can prescribe pills that will kill the fungus.
If ringworm is not treated, your skin could blister, and the cracks could become infected with bacteria. If this happens, you will need antibiotics. If your child is being treated for ringworm, you don't have to keep him or her out of school or day care.
Scabies is an itchy skin condition caused by a tiny, eight-legged burrowing mite called Sarcoptes scabiei. The presence of the mite leads to intense itching in the area of its burrows. The urge to scratch may be especially strong while you're in bed at night.
Scabies is contagious and can spread quickly through close physical contact in a family, child care group, school class or nursing home. Because of the contagious nature of scabies, doctors often recommend treatment for entire families or contact groups to eliminate the mite.
Medications applied to your skin kill the mites that cause scabies, although you may still experience some itching for several weeks.
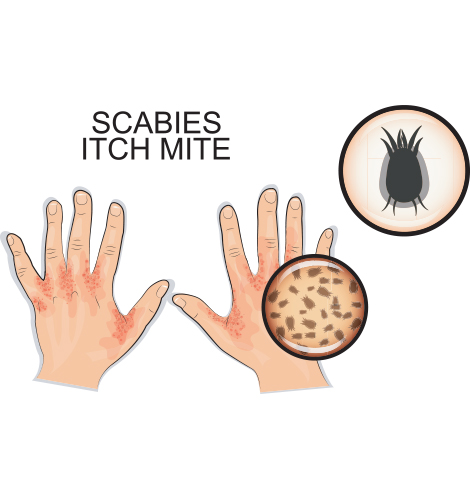

Scabies symptoms include:
1. Itching, often severe and usually worse at night.
2. Thin, irregular burrow tracks made up of tiny blisters or bumps on your skin.
To diagnose scabies, your doctor examines your skin, looking for signs of mites, including the characteristic burrows. When your doctor locates a mite burrow, he or she may take a scraping from that area of your skin to examine under a microscope. The microscopic examination can determine the presence of mites or their eggs.
Scabies treatment involves eliminating the infestation with medications. Several creams and lotions are available. You usually apply the medication over all your body, from your neck down, and leave the medication on for at least eight hours. Two medications commonly prescribed are permethrin and crotamiton. Although these medications kill the mites promptly, you may find that the itching doesn't stop entirely for several weeks.
Doctors sometimes prescribe oral medications for people with altered immune systems or for people who don't respond to the prescription lotions and creams.
Because scabies spreads so easily, your doctor may recommend treatment for all family members and other close contacts, even if they show no signs of scabies infestation.

To prevent re-infestation and to prevent the mites from spreading to other people, take these steps:
1. Clean all clothes and linen. Use hot, soapy water to wash all clothing, towels and bedding you used at least two days before treatment. Dry with high heat. Dry-clean items you can't wash at home.
2. Starve the mites. Consider placing items you can't wash in a sealed plastic bag and leaving it in an out-of-the-way place, such as in your garage, for a couple of weeks. Mites die if they don't eat for a week.